Snoring and Sleep Apnoea
What Causes Snoring?
Snoring occurs when the soft tissue structures of the upper airway collapse onto themselves and vibrate against each other as we attempt to move air through them. This produces the sound we know as snoring. Large tonsils, a long soft palate, a large tongue, the uvula, and excess fat deposits in the throat all contribute to airway narrowing and snoring. Usually, the more narrow the airway space, the louder or more habitual the snoring.

Snoring Relation to Sleep Apnoea
Snoring is the sound of partially obstructed breathing during sleep. While snoring can be harmless, it can also be the sign of a more serious medical condition known as Obstructive Sleep Apnoea (OSA).When Obstructive Sleep Apnoea occurs, the tongue and soft palate collapse onto the back of the throat and completely block the airway, which restricts the flow of oxygen. The condition known as Upper Airway Resistance Syndrome (UARS), is midway between primary snoring and true obstructive sleep apnoea. People with UARS suffer many of the symptoms of OSA but require special sleep testing techniques.
What is Sleep Apnoea?
OSA is a serious and relatively common condition. 750,000 Australians have problems with their health due to OSA.
- Sleep Apnoea has been linked to:1-3
- High blood pressure
- Diabetes
- Heart failure
- Car and truck accidents
- Work accidents
- Stroke
There are two main types of sleep apnoea; obstructive sleep apnoea and central sleep apnea*. 85% of people with sleep apnoea have obstructive sleep apnea. This is caused by the muscles in the back of your throat relaxing and interfering with your breathing while you sleep. 5
Obstructive sleep apnoea can have a number of warning symptoms, including daytime sleepiness or tiredness, weight gain and decreased sex drive.
The good news is that successful OSA treatment can help alleviate the symptoms and reduce the long-term risks to your health.6
Causes of Sleep Apnoea
When you go to sleep, the muscles at the back of your throat relax. When this happens, your airway can narrow or close as you breathe. Because your airway is partly blocked, snoring results. If the airway becomes completely blocked, you can’t get any air into your lungs.
Normal Airway
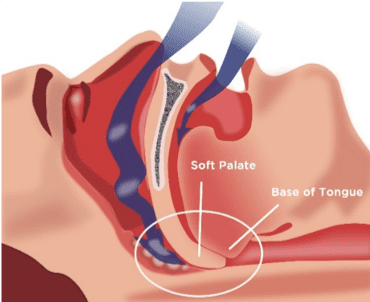
Obstructed Airway
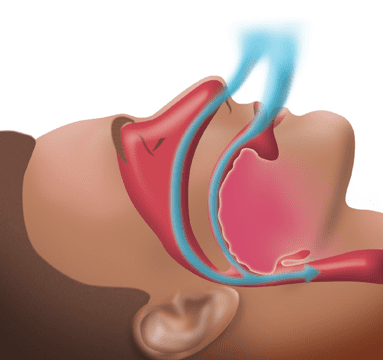
Oral Appliance
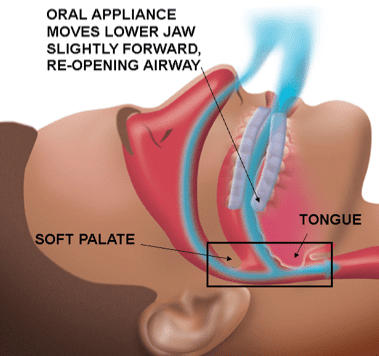
This can happen many times a night without you being aware of it. You may think you slept all night. Obstructive sleep apnoea causes poor quality sleep and often results in sleepiness during the day.¹ Your brain responds to the low oxygen level in your blood by briefly waking you from sleep so that you can take a breath. Your partner may notice that you make a gasping or choking sound.1
You can find out if you have sleep apnoea, by having a sleep assessment.
*Central sleep apnoea is a less common form of sleep apnoea. It is caused by the brain failing to send the right signals to the muscles that control breathing. Some people have ‘complex’ sleep apnoea, which is a combination of obstructive and central sleep apnoea. A sleep assessment will determine whether you have these conditions.4
Sleep Apnoea Signs and Symptoms
Apart from snoring (and the relationship problems that can go with it), the first sign of obstructive sleep apnoea (OSA) that many people notice is nodding off in the daytime — in front of the TV, at work or on public transport.
Others catch themselves nodding off behind the wheel, an event that becomes a literal wake-up call that something is very wrong.3
Sleep apnoea can reveal its presence in a number of ways, and each patient may have a unique combination of symptoms. If you experience any of the following recurring: 7
- Excessive daytime sleepiness
- Morning Headaches / Migraines
- Snoring
- Weight Gain
- Short Term Memory Problems/ Forgetfulness
- Acid Reflux
- High Blood Pressure
- Depression
- Severe Anxiety
- ADD & ADHD Symptoms
- Choking/Gasping sensation that wakes you up
- Insomnia / Inability to sleep through the night
- Diabetes
- Sore Throat / Dry Mouth
- Slow Metabolism / Inability to lose weight
- Poor job performance or problems in school
- Mouth Breathing /Difficult Nose Breathing
- Restless and tossing and turning during sleep
- Impotence and/or Decreased Sex Drive
- Mood Swings / Temperamental Behaviour
- Poor concentration
- High blood pressure
- Lack of energy
- Night sweats
- Frequent urination at night
Diagnosis
Since OSA is a serious medical condition, it must be diagnosed by a physician. Once a diagnosis of sleep apnoea is made, the severity of the dysfunction can be classified and treatment options will be given.
Sleep Studies
A sleep study gives the best picture of how you breathe when you sleep. It provides information regarding apnoeas (when breathing stops) and hypopneas (when breathing is shallow due to an obstruction) as well as pulse, blood pressure and other physiological processes such as REM sleep, EEG and leg or arm jerking. Depending on your circumstances, Dr. Willey will recommend either a PSG or a HST.
Polysomnogram (PSG)
A PSG is a sleep study that is done in a sleep lab overnight and monitored by a trained sleep lab technician. The patient is hooked up with wires via sticky electrodes to the apparatus that will monitor their sleep channels. The physician associated with the sleep lab will examine the results and interpret the data collected.
Home Sleep Test (HST)
An ambulatory sleep study, or HST, is a convenient monitoring system that the patient can use in the comfort of his own bed. The HST is a small, portable unit that utilizes wireless technology. The data recorded during sleep is then downloaded to a computer the next day. This data is analysed by a certified sleep physician.
